Cancer is the second cause of death, right after cardiovascular diseases (such as strokes and heart attacks) in most developed countries.
Cancer is a dreadful disease. In my new, upcoming book on longevity, I explain how cancer originates and how to better treat and prevent it.
But detecting cancer at an early stage is also a very important aspect of not dying from cancer.
Current cancer treatments are very taxing and detrimental to the body, not only damaging cancer cells, but also healthy cells and tissues, as happens with chemotherapy, radiation and surgery.
Therefore, it’s crucial to prevent cancer, and if it does arise, to detect cancer early, so the patient has a much better likelihood of being cured.
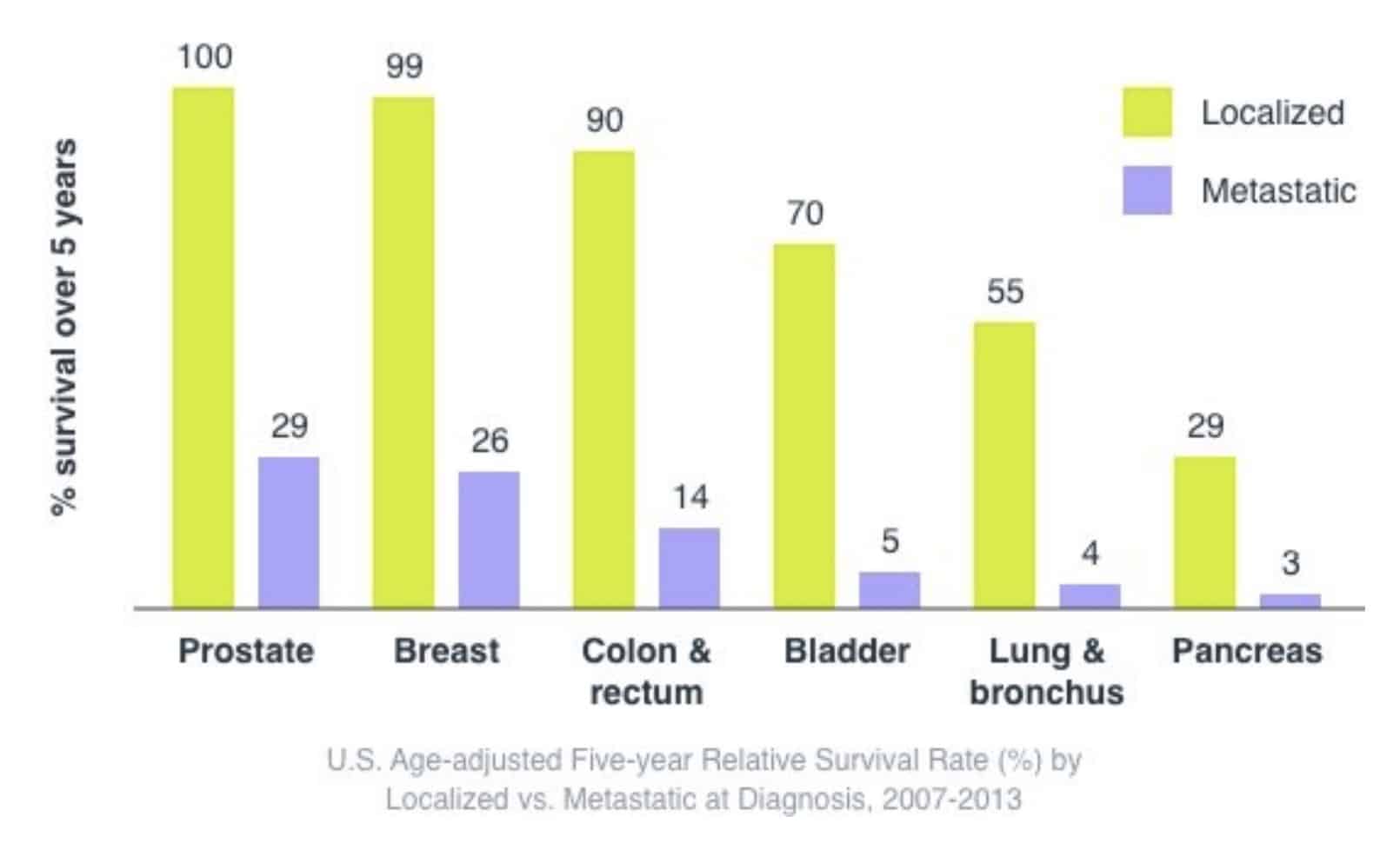
When a cancer is diagnosed early, before it has had the chance to spread, the 5-year survival rate is 4 times higher than when diagnosed at a later stage:
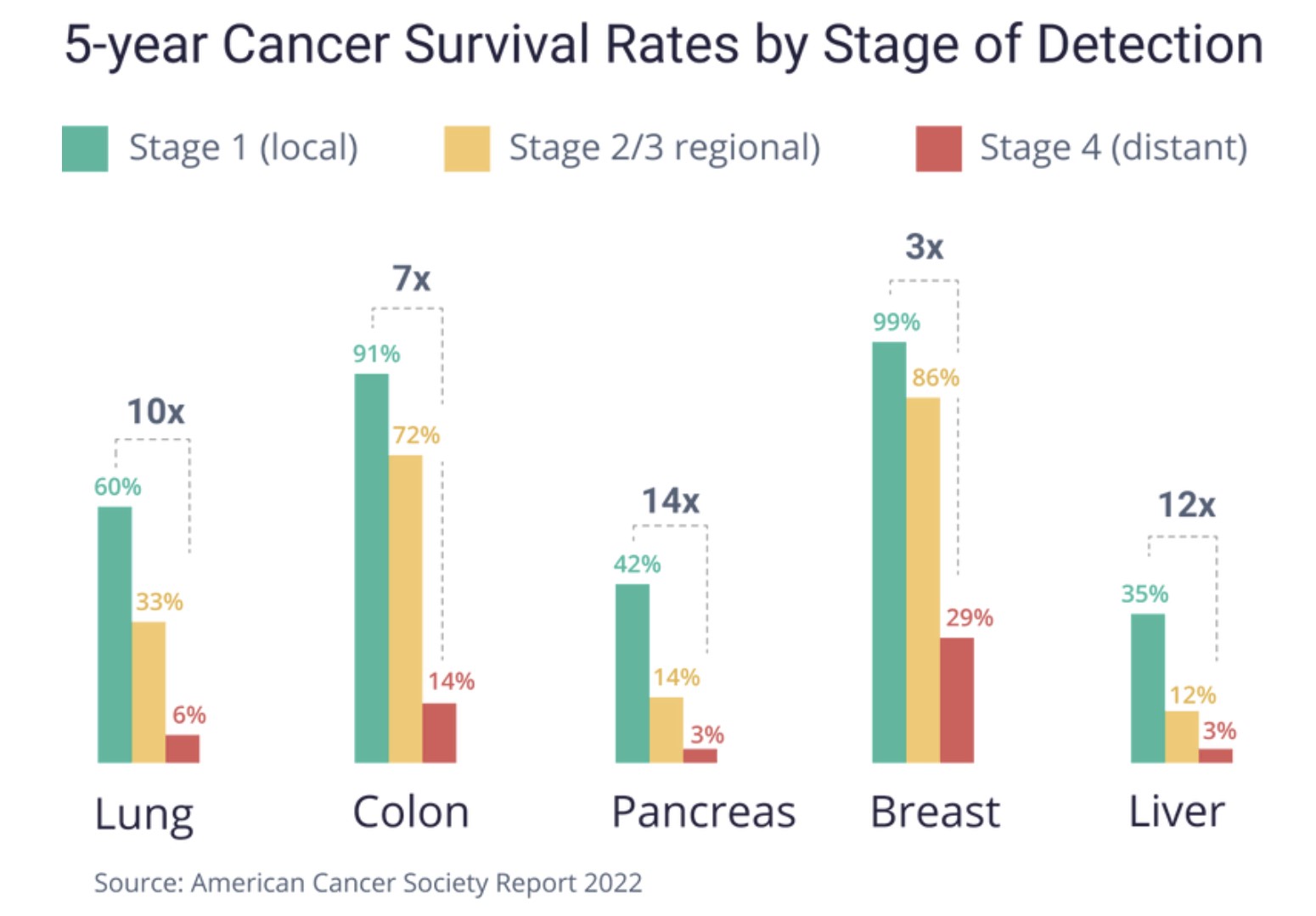
For various cancers, chances of survival are more than ten times higher when detected at an early stage (stage 1) versus a later stage (stage 4), especially for liver, lung and pancreas cancer:
To screen for cancer, there exist two main categories of tests:
– Multi-cancer early detection tests: which screen for multiple cancers at the same time. An example is the Galleri test.
– Single-cancer early detection tests: these tests focus on one specific kind of cancer, like colon cancer or cervix cancer.
Let’s start with multi-cancer early detection tests (MCEDS).
Multi-cancer early detection tests (MCEDS)
These tests screen for multiple cancers. A blood sample is drawn. This test looks for traces of cancer, such as circulating tumor DNA, which is DNA that tumor cells release into the blood.
This circulating DNA coming from cancer cells is somewhat mutated, or has epigenetic changes, meaning it’s methylated differently (different arrangements of methyl groups on the DNA) or is histonylated differently (the DNA is wrapped differently around histones, which are proteins around which the DNA strand is wrapped).
Specific diagnostic machines can measure this mutated, cancer-derived DNA from a blood sample. Some tests also look at other substances which cancer cells secrete, like specific proteins, peptides (fragments of proteins) or RNA.
Artificial intelligence is also often used to detect this circulating tumor DNA, proteins and RNA to diagnose cancer at a much earlier stage.
An example of such a multi-cancer detection test is the Galleri test. This cancer screening test claims to “screen for more than 50 cancers”.
This sounds impressive, but there are various things to take into account when assessing such multi-cancer screening tests.
Let’s take the Galleri test as an example, and what to take into account to see how good such a test really is to track down cancer much earlier.
1. Multi-cancer screening tests do not screen for all cancers
The Galleri test screens for 50 cancers. This sounds formidable. However, there are many cancers. In fact, there are literally hundreds of different types of cancers.
The Galleri test does not screen for many other cancers. For example, the Galleri test does not screen for various brain cancers because they shed limited amounts of tumor DNA into the blood.
2. The sensitivity of the test depends on the type of cancer
The Galleri test cannot detect all cancers with the same high accuracy. It can detect some cancers (much) better (or worse) than others. So its “sensitivity” can differ wildly for the 50+ cancers this test can “detect”.
“Sensitivity” means the ability of a test to correctly diagnose people with cancer (these people are called “true positives”, so people who have cancer).
The higher the sensitivity of a test, the better. For example, a test with a sensitivity of 98% means that the test will detect 98 (true positives) out of 100 people with cancer, missing only 2 people with cancer (false negatives).
The Galleri test has different sensitivities for different types of cancer. Galleri’s sensitivity for some cancers is very low, meaning it’s not good at detecting these cancers.
These are cancers like prostate cancer (a very prevalent cancer in older men), kidney cancer, bladder cancer, breast cancer (the most common cancer in women), and myeloid cancer, among others.
The sensitivity for prostate cancer is only 11.2%, which means this test misses 88.8% of people who have prostate cancer. The sensitivity for bladder cancer is 34.8%, meaning it misses two third of people with bladder cancer (see figure below):
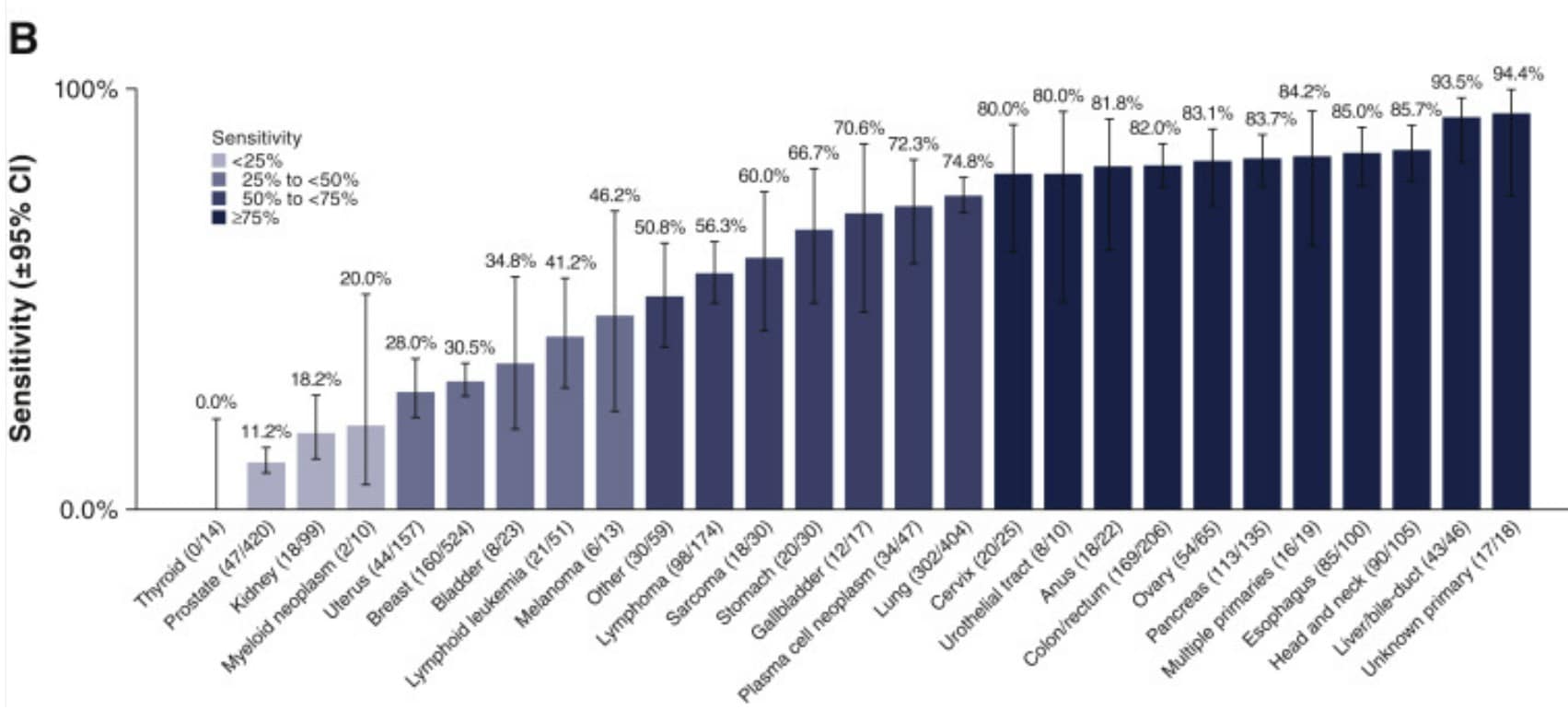
With such low sensitivities, screening for these cancers is quite useless for doctors; you don’t want a test that misses two thirds or even half of all cancers. For a screening test to be acceptable, the sensitivity should be at least 80%, and ideally more than 90%.
The overall sensitivity of the Galleri test was 52%. This is when taking all cancers together and calculating the average sensitivity. This means this test can detect about half of these cancers in people.
For some cancers, its sensitivity is much higher, more than 80% for ovary cancer, colon cancer, esophageal cancer, liver and bile-duct cancer for example. But as discussed, for various cancers, its sensitivity is too low.
Therefore, it’s important to always combine a multiple-cancer screening test like Galleri with other tests that have a much higher sensitivity for specific cancers. I will discuss these tests later on.
3. Less good at detecting early-stage cancers
The sensitivity of a test also depends on the stage of the cancer. Early-stage, smaller cancers are of course less easy to detect than later-stage, larger cancers.
This is a problem, given that we want to detect cancers as early as possible given that the success of a treatment is then much higher.
For the twelve cancers the Galleri test is best at screening for, such as lymphoma, esophageal, colorectal, anal, stomach, liver/bile-duct, ovary, pancreatic, plasma-cell, bladder, lung cancer, the Galleri tests finds only about 40% of stage I cancers, 67% of stage II cancers, 80% of stage III cancers and 95% of stage IV cancers.
So for early stage cancers, it misses more than half of these cancers (actually, 60%). Of course, better to detect cancer at a later stage than not detecting it at all.
Conclusion
Does this mean that a test like the Galleri test is not recommended? The Galleri test can be a useful screening test. But it still has lots of shortcomings, like not screening for al cancers, having only acceptable sensitivity for some cancers, and being less able to detect early stage cancer.
Nonetheless, this test good at screening cancers like liver cancer, bile-duct cancer, neck cancers, esophagus cancer, pancreas cancer, ovary cancer, colon and rectum and anal cancer, cervical cancer, cancers of the urine tract, with sensitivities of more than 80%, especially for later stage cancer.
But for many other cancers, such as prostate cancer and kidney cancer, its sensitivity is too low.
Therefore, tests like the Galleri test should always be combined with other screening tests and methods.
Of course, this will change. The scientists who developed the Galleri test will further improve this test. Many other researchers and companies are working on similar early cancer screening tests. Examples are Freenome, Inivata, Accuragen, Diagu, and many others.
Scientists are looking not only for for mutated circulating tumor DNA (ctDNA), but also changes in the epigenome of circulating cancer DNA strands, while also using proteomics (detecting specific proteins and peptides released by cancer cells), transcriptomics (RNA strands released by cancer cells into the blood), and apply ever more sophisticated machine learning algorithms to detect patterns that will allow diagnosing cancer much sooner and with higher sensitivity.
Imagine a future where people go to their doctor (or order a test at home), and provide a little bit of blood (or urine in case of prostate cancer), which is then sent to a lab to be analysed to detect cancer much earlier so people can be treated far more successfully. This is a future we are heading to.